The International Labor Organization estimates that globally, 2.78 million people die each year from causes attributed to work. Fatal accidents accounted for 13.7% of these deaths but surprisingly, the vast majority of these deaths, 2.4 million or 86.3%, were due to work-related diseases. Circulatory conditions, work-related cancers, and respiratory diseases were the top three diagnostic categories.
Understandably, many have asked how experts determine that a condition is work-related since occupational diseases often have a long latency period and may not be clinically or pathologically different than non-work-related diseases. While the work relatedness of some occupational diseases is well known (e.g., mesothelioma or silicosis), linking other diseases to the workplace often requires a more in-depth analysis.
From a population perspective, experts use epidemiological methods to determine the proportion of occupational disease related to a specific risk factor. By extension, with certain caveats, this attributable fraction can also be used to estimate the fraction of disease that would not occur if exposure to the risk factor was not present. These kinds of studies are instrumental in prompting further research into the mechanism of disease causation and development of effective treatment regimens.
When attempting to diagnose an occupational disease in an individual, clinicians need to follow a stepwise approach that begins with taking a full clinical history, which should include relevant information regarding the patient’s occupation. The association with the workplace must then be evaluated in the context of the following:
- Is there a known linkage between the condition and risk factors in the workplace?
- Is there an identifiable dose-response relationship?
- Does the temporal relationship add further support for work relatedness?
- Are there other more likely causes for the condition in question, such as underlying conditions, lifestyle (e.g., smoking), family history, etc.?
The health and wellbeing of employees is truly a valuable asset and occupational disease exacts an unmeasurable emotional and financial toll on all involved—employers, workers, and their families. Leaders in occupational medicine have a duty to not only treat these diseases but should work with employers to prevent them from occurring—especially across various global work locations where protective regulations may not exist. Below are suggestions to help you design workplace programs that will put you on a journey toward prevention and actively demonstrate your commitment to worker safety and health.
Know Your Workplace
The occupational medicine professional should be familiar with the chemical, physical, biologic, and other hazards present in their workplace. Examples of these are listed below.
- Chemical hazards such as gases, liquids, dust/fibers (silica, asbestos, man-made fibers, etc.), welding fumes, and selected pharmaceutical agents
- Physical hazards such as ionizing and non-ionizing radiation, electromagnetic fields, noise, temperature extremes, and emerging risks such as sedentary work
- Biologic hazards such as selected viruses (hepatitis B, C) and pharmaceutical agents
You should comply with local regulations, which may specify exposure limits, required exams, and special treatment of vulnerable populations.
Walk through your work areas to observe the interaction between workers and the environment to determine:
- Are workers potentially exposed to one or more hazards? Have exposure levels been accurately measured under true working conditions?
- Is appropriate personal protective equipment (PPE) available?
- Do individuals receive training on the proper use of PPE?
- Is the use of PPE enforced in areas where there is potential for exposure?
Be responsive to employee concerns by
- Ensuring that employees have access to basic information regarding workplace exposures and protective measures
- Establishing a mechanism via which employees can report concerns and be referred for further assessment as needed
Utilize a Hierarchy of Controls
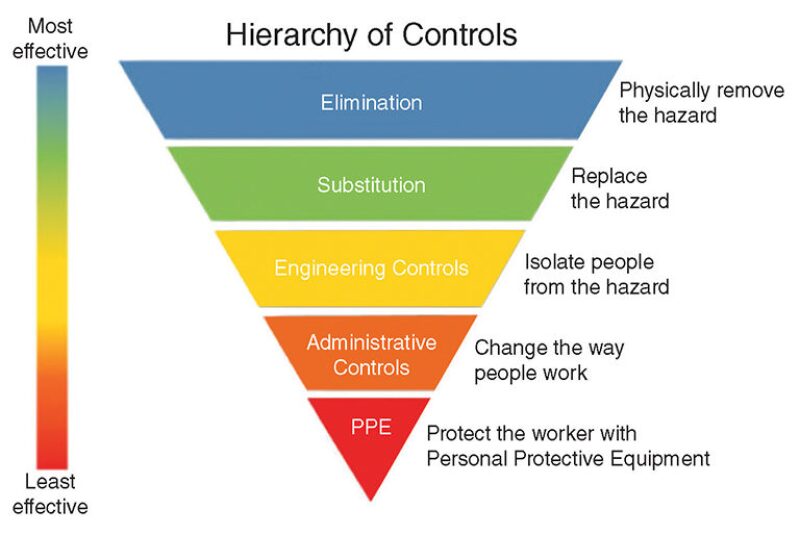
Once potential hazards are identified you can use a Hierarchy of Controls framework to determine the best approach to control the hazards of concern (Fig. 1). Starting at the top of the pyramid, the control options are arranged from most to least effective. It is important to note that hazard elimination is the most effective control measure while PPE use is the least effective since its effectiveness depends on the ongoing efforts of individuals. To learn more about these hazard control solutions, go to the Centers for Disease Control and Prevention website at www.cdc.gov/niosh/topics/hierarchy/default.html.
Consult an Occupational Health Specialist
If the exposures in your workplace are numerous or comprise complex mixtures, it may be prudent to consult a trained occupational medicine consultant. This consultant can utilize industrial hygienists to characterize the various workplace exposures, advise you of any applicable regulatory requirements, propose feasible control options, and provide recommendations for any ongoing monitoring. Skilled consultants should also be able to utilize the National Institute for Occupational Safety and Health Total Worker Health principles to develop a more integrated and holistic approach to workplace health and safety.
Additionally, if “at risk” workers are discovered, an occupational medicine physician may propose a health surveillance program wherein potentially exposed workers are periodically examined to determine the need for further evaluation, medical treatment, and/or removal from exposure.
